HEALTH EQUITY
Health equity is the attainment of the highest level of health for all people in a community, valuing everyone equally. Health equity means a focused and ongoing effort to address avoidable socioeconomic inequalities in health, healthcare and community development.
Contact: Devin Thompson
Building wealth isn’t just about saving money or improving access to lending. Economic well being is intrinsically tied to social, physical and mental health, and financial instability has a direct ramification on a person’s health.The connection between health and community development is clear. Low- to moderate-income communities tend to suffer much more from health issues than wealthier neighborhoods. And health inequality prohibits many families and individuals from generating wealth.
Get the Health & Wealth Newsletter
Utilizing our model of community reinvestment organizing, NCRC encourages banks to support more holistic and inclusive community development efforts. Analogously, we also collaborate with organizations and members to bring together these same financial institutions with health care systems.
Through research and listening sessions, NCRC has observed that the underpinning of an individual’s health is the ability to maintain safe and affordable housing. NCRC values the opportunity to collaborate with our members, community stakeholders and hospitals and health systems as we strive to improve the health of our communities and its most vulnerable members. By improving health, we can make strides toward a more just economy.
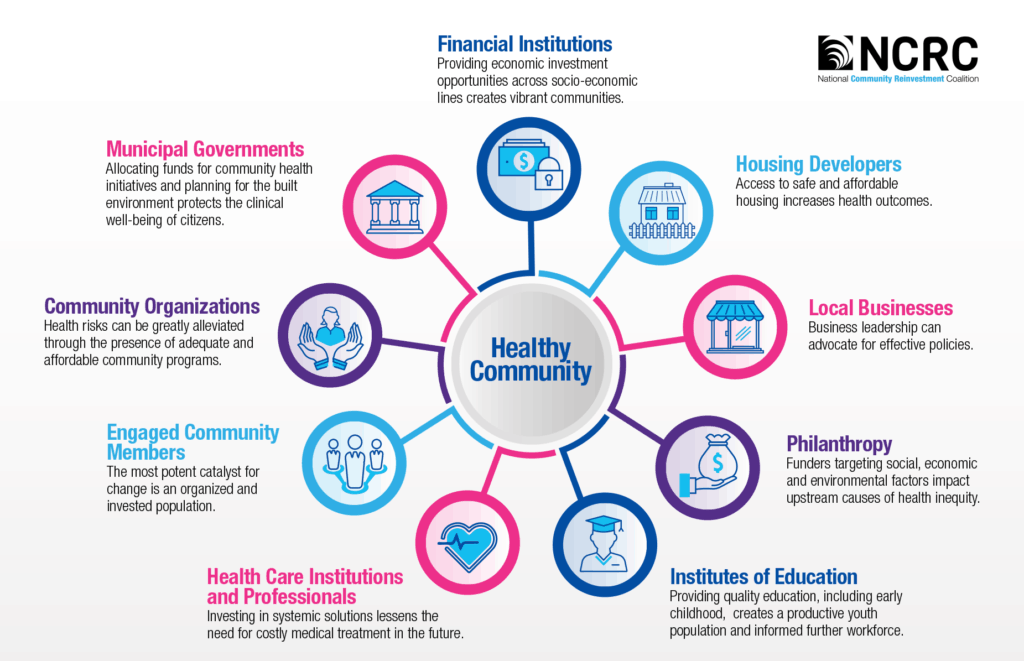
Our Model of a Healthy Community
Webinar
Healthy Communities – Partnering with Hospitals to Invest in Community Development
Related Items:
Healthy Communities – Partnering with Hospitals to Invest in Community Development (Webinar)
Wealth equity includes health equity
Low-income housing: The negative effects on both physical and mental health
There is no wealth without mental health
Latest

Health Equity Research Spotlight: Challenges And Solutions For Connecting Community Development And Public Health Institutions
Two recent studies of health equity work show the challenges that community development and public health organizations face in building trust.
Health Equity Research Spotlight: Housing Vouchers Improve Physical Health
Public health outcomes improve when HUD housing vouchers are more widely available.

“Weathering” And The Effects Of Racism On Public Health
Public health and health equity experts often refer to the concept of “weathering.” So what is it?

Loss Of Medicaid Coverage Disproportionately Impacted People Of Color
A process known as “Medicaid unwinding” is dumping tens of millions of low-income households off a key anti-poverty program, usually without solid evidence.

Study Finds Socioeconomic Conditions – Not Genetics Or Lifestyle Choices – Account For Racial Life Expectancy Gap
There is a large and persistent racial life expectancy gap in the United States. And it isn’t happening because of lifestyle choices.

HEALTH EQUITY RESEARCH SPOTLIGHT: Medical Debt Makes People Live Sicker, Die Sooner
Owing someone money doesn’t just make a person’s life harder – it might also make it shorter, and it certainly makes it sicker.

Understanding The Dire Economic And Health Inequities Facing Transgender Americans
In recognition of Pride Month this June, this piece details the special threats to health equity that haunt the transgender community.

Partnering For Health Equity At The 2023 Just Economy Conference
How can community development organizations collaborate with health care providers to promote equity?